If you are struggling with the appearance of your chest, the first and most important step is to get a clear, medical diagnosis. Many men feel self-conscious about this, but it’s crucial to know that “man boobs” are a recognised medical condition, not a personal failing.
Understanding what gynecomastia is—and what it isn’t—is the foundation for finding the right, permanent solution. Gynecomastia is one of the most common disorders affecting adolescent and adult males.
The first step toward effective Gynecomastia Treatment in Jaipur is understanding precisely what the condition is. If you are experiencing uncomfortable enlargement of the male chest, rest assured that this is a recognised medical condition.
True Gynecomastia Definition
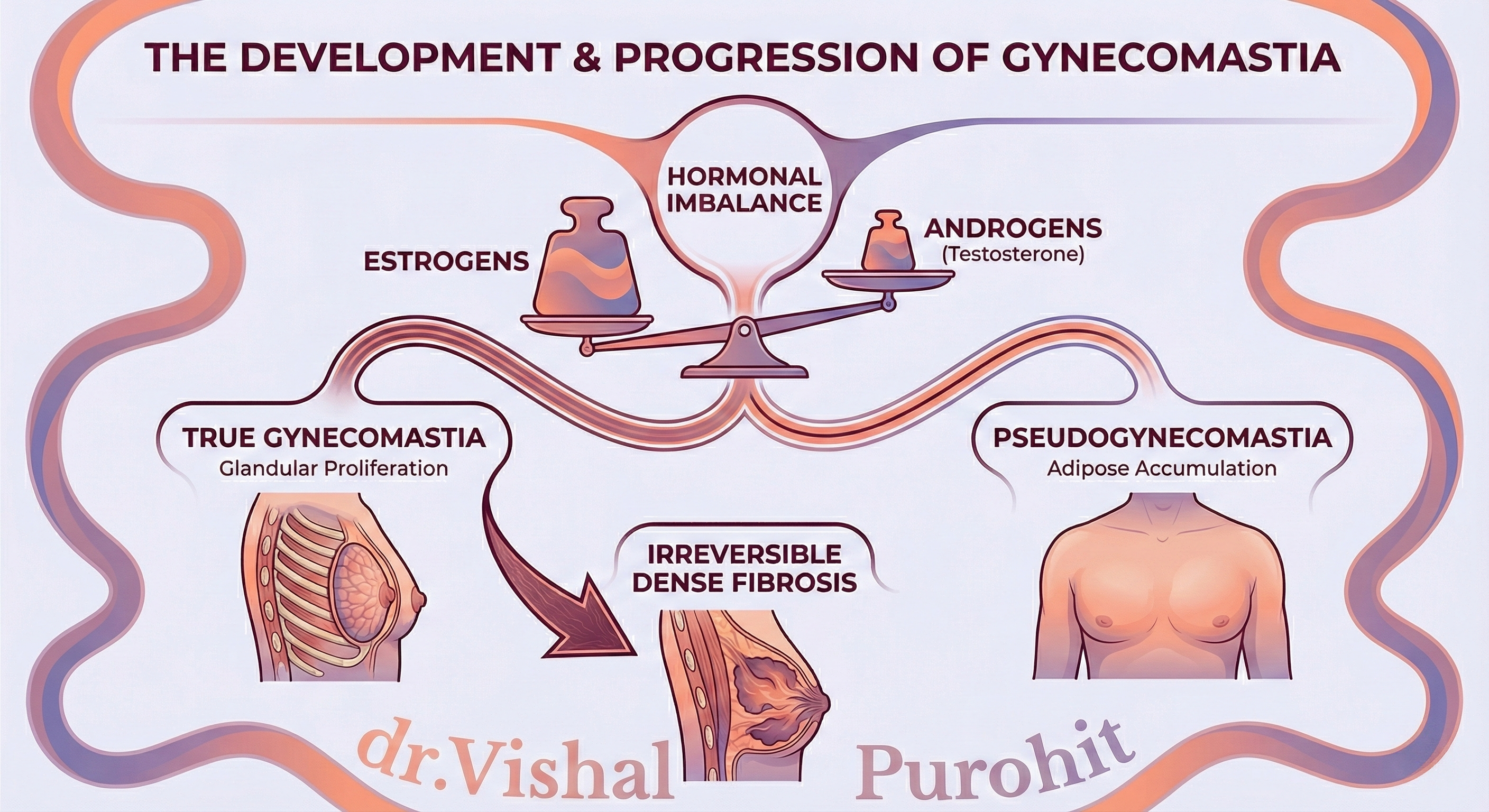
True gynecomastia is defined as the benign proliferation of glandular breast tissue, characterised by a firm disc of tissue underlying the nipple. This glandular tissue is often firm and rubbery because it is composed of ductal and stromal tissues that can progress to irreversible dense fibrosis and hyalinization.
If the gland progresses to dense hyalinized fibrous tissue, medical therapy is ineffective, and surgical correction is indicated.
Gynecomastia is a common condition affecting many men.
In simpler medical terms, gynecomastia is the non-cancerous (benign) enlargement or overdevelopment of one or both breasts in men.
It is also called “man boobs” or “moobs”.
This enlargement is the result of a hormone imbalance between estrogens and androgens (testosterone). Specifically, it results from a disparity between estrogen and testosterone, or an altered ratio of estrogens to androgens.
Pseudogynecomastia (Lipomastia) Definition:
Pseudogynecomastia represents excessive accumulation of soft, ill-defined adipose (fat) tissue on the chest wall, without glandular proliferation.
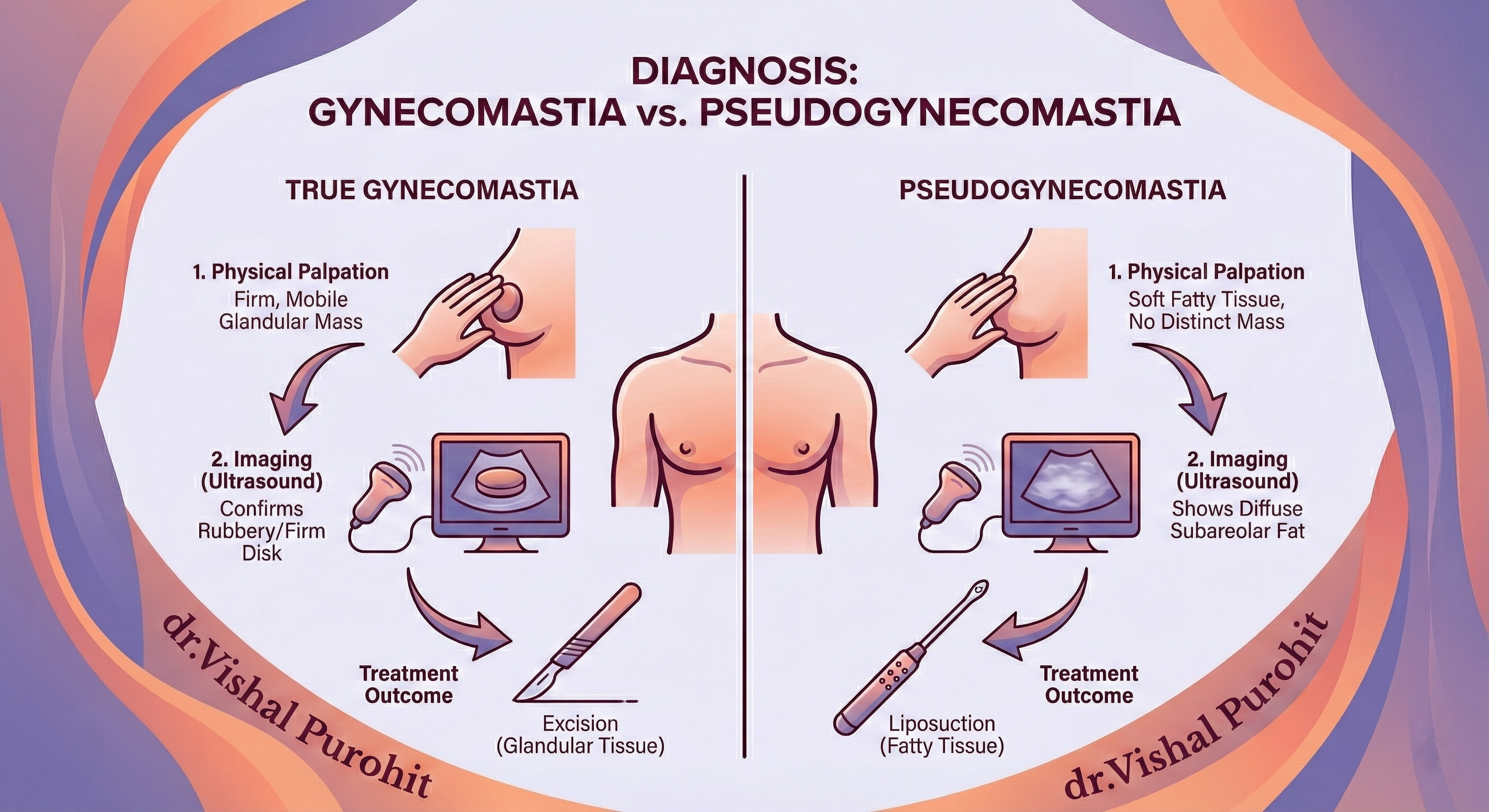
The Nuance in Diagnosis: gynecomastia vs pseudogynecomastia
Physical Palpation:
The diagnosis is not based purely on appearance; it requires a physical examination by an experienced surgeon to determine the underlying tissue type.
True gynecomastia is characterised by a soft, compressible, and mobile mass of breast tissue felt under the nipple and its surrounding skin. This is in sharp contrast to softer fatty tissue, which is not associated with a distinct mass. Your surgeon will examine you thoroughly and may suggest imaging tests like an ultrasound or mammography to confirm the diagnosis, if necessary.
This diagnosis is the first step before determining the grade of your condition, which dictates the surgical approach. For cases where fat is the main concern (Pseudogynecomastia), the liposuction technique is used. However, if true glandular tissue is present (true gynecomastia or mixed gynecomastia), excision is required to achieve a permanent solution.
Imaging:
While palpation is crucial, the diagnosis can be confirmed by imaging. In true gynecomastia, a rubbery or firm disk is palpated under the nipple–areola complex, but in pseudogynecomastia, such disks were not palpated.
It is often more correct to refer to cases as gynecomastia with a prevalent glandular component or a prevalent adipose component rather than purely glandular or purely fatty forms.
Gynecomastia is a unilateral or bilateral mammary gland hyperplasia in men that is benign and not reversible, often confused with pseudogynecomastia, which refers to subareolar fat accumulation without gland involvement.
Spectrum of Physical Presentation Increases Discomfort
The physical presentation of gynecomastia varies widely.
The condition can be a little conical protrusion appearing like a puffy nipple, to a fully developed breast like a female.
Regardless of severity, it often carries a significant emotional weight. It causes emotional discomfort, anxiety, and social stigma. It impairs self-confidence, often leading men to avoid social gatherings, the gym, swimming, or wearing well-fitted clothes.
Pathogenesis: Why the Chest Enlarges in Gynecomastia
Gynecomastia results from an absolute or relative imbalance between estrogens (which stimulate breast development) and androgens (which antagonise this effect).
This condition typically occurs in three distinct phases of a man’s life:
1. Neonatal Period: Highly prevalent (60–90% of infants) due to high maternal estrogen levels.
2. Adolescence/Puberty: Common (30–65% of boys). Although most cases resolve spontaneously within two or three years, persistence into adulthood in roughly 8% of patients has been reported.
3. Elderly/Ageing (50–80 years): Prevalence increases significantly, reaching up to 70% in men aged 50–69 years.
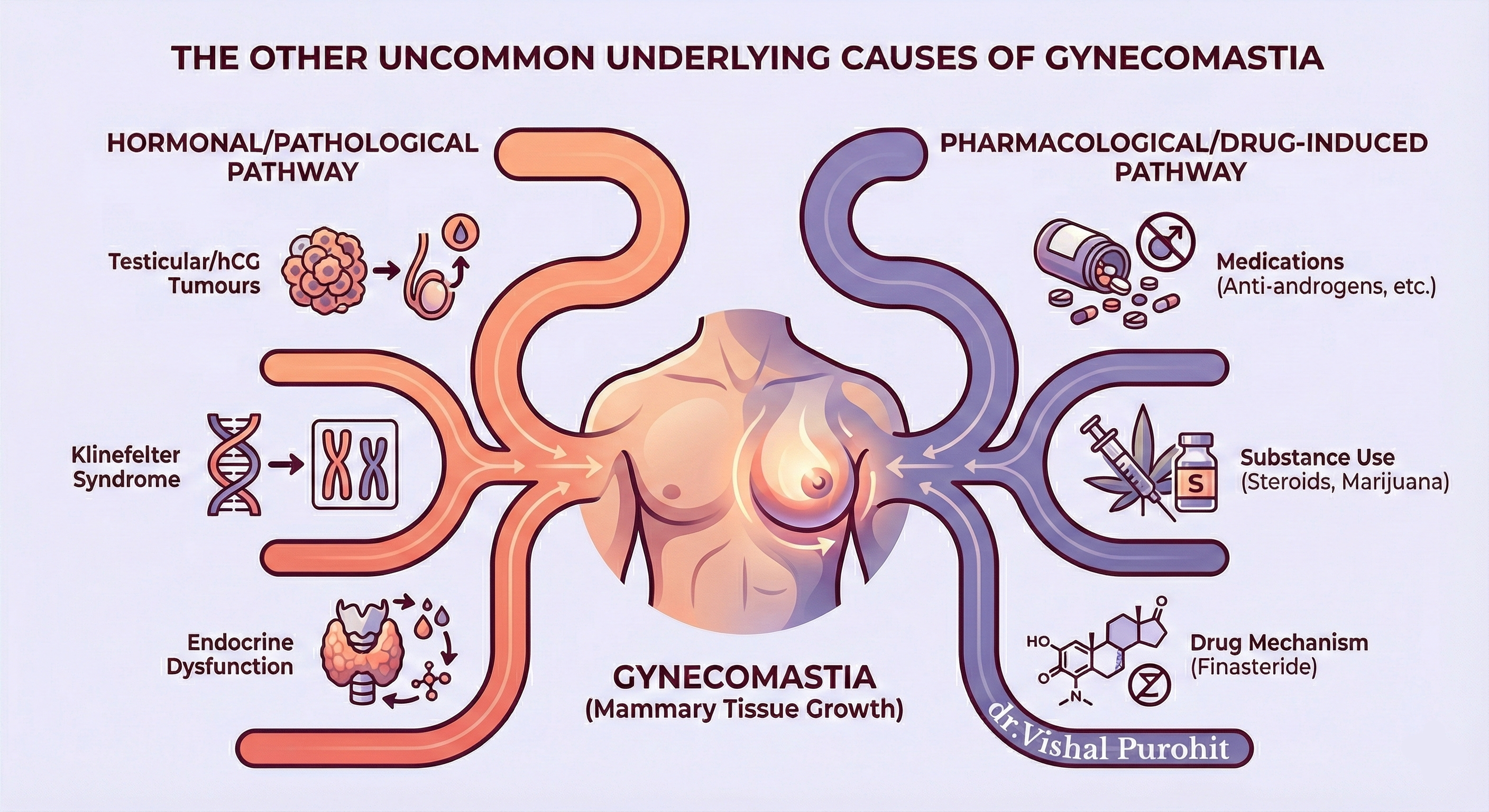
The Other Uncommon Underlying Causes of Gynecomastia
The aetiology of gynecomastia contains a wide spectrum including physiologic, endocrinologic, metabolic, neoplastic, and drug-induced causes.
Hormonal/Pathological Causes
The hormonal imbalance can be due to systemic disorders, endocrine issues, or tumours:
- Endocrine Dysfunction: The imbalance can stem from conditions like testicular estradiol production (tumours), Klinefelter syndrome, or drugs.
- Klinefelter Syndrome: This syndrome represents a very important subset of patients because they carry a dramatically increased risk of breast carcinoma.
- Tumours: Testicular tumours and hCG-secreting tumours must be excluded by ultrasound examination, even if the clinical exam is normal.
Pharmacological/Drug-Induced Causes
A significant number of cases are due to medications or substance use that disrupt the estrogen/androgen balance.
- Drug Mechanism: Drugs like finasteride inhibit 5a-DHT, which increases estradiol levels, thought to stimulate mammary tissue growth.
- Substance Use: Anabolic steroids, marijuana, or alcohol abuse are implicated.
- Medications: Medications implicated include anti-androgens, anti-ulcer drugs, anti-retrovirals, and specific psychotropic agents, highlighting the importance of a thorough patient history and discussion of drug-induced gynecomastia.
Idiopathic Causes
The cause is unknown or cannot be attributed to a specific disorder in about 25% of cases.
Special Nuances in Diagnosis
Asymmetry: Although most cases are bilateral, gynecomastia can present as unilateral. The clinical characteristics of asymmetric bilateral gynecomastia (ABGM) require careful evaluation.
Complicated Forms: Some forms of gynecomastia do not match properly the existing classifications, requiring specialised diagnosis. The quality of the skin represents a crucial element for the surgical strategy
Your Consultation in Jaipur
Your specific diagnosis determines the best permanent solution. To receive a professional physical exam and definitively diagnose the nature of your breast enlargement, I invite you to a private consultation.
To book your personalised, confidential consultation, please reach out to my team at Kalpana Aesthetics.
- Call or WhatsApp: 7718183535
- Visit Us: Kalpana Aesthetics, 2nd Floor, Jaipur Hospital, Mahaveer Nagar, Tonk Road, Jaipur
Disclaimer: The information provided on this webpage is for educational purposes only and does not constitute medical advice. The content is not intended to be a substitute for professional medical diagnosis or treatment. Please consult with a qualified, board-certified plastic surgeon to discuss your specific condition.

